|
Source : Daily Mail Ditch the paracetamol and try ACUPUNCTURE: Scientists prove it can rewire the brain and make the body better able to cope with pain.
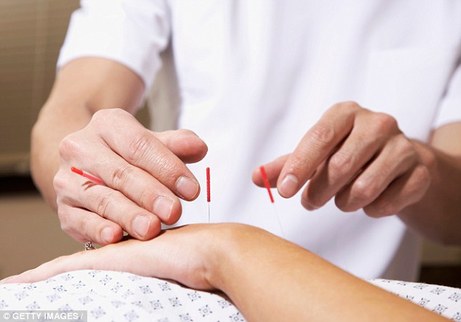
Acupuncture can be used to relieve pain in sufferers of repetitive strain injuries, new research suggests. Currently patients with carpal tunnel syndrome - common in office workers - undergo physiotherapy or surgery to assist them. It is caused by a nerve in the wrist being squeezed and subsequently alters an area of the brain related to touch, scientists claim. But the new study found the ancient Chinese practice rewires the brain and helps to combat the aching and tingling sensations. Participants were given brain scans after receiving electro-acupuncture - similar to the traditional method but instead uses electricity to generate impulses - on their affected hand. They were also assessed by Massachusetts General Hospital researchers after having the same treatment on their ankle opposite their injured hand. Others received 'sham' acupuncture - where placebo needles were placed near their affected region. While he also noted that the treatment method helps to increase blood flow to the affected areas, known to fight discomfort. However, the sham treatment method could work through the placebo effect, he added. Dr Napadow said: 'Acupuncture is a medical therapy that originated in China several thousand years ago. 'But despite its long history, the intervention itself - particularly when coupled with electrical stimulation - has significant similarities to many conventional therapies. 'A large body of clinical research exploring acupuncture for chronic pain disorders has demonstrated that it may be marginally better than a placebo procedure in reducing pain ratings.' This comes after a report in January claimed that acupuncture could help men with premature ejaculation. Scientists from the University of Sheffield found that Chinese herbal medicine and a Korean topical cream both had significant desirable effects. While a study last month also discovered that acupuncture could stop babies suffering from colic from crying so much. The Swedish researchers noted that the practice could help to reduce the distress of babies with the condition. Read more: http://www.dailymail.co.uk/health/article-4274898/Ditch-paracetamol-try-ACUPUNCTURE.html#ixzz4aYGd3Cgf The hay fever season is just around the corner so, if hay fever is something that has troubled you over the years, maybe give acupuncture a try. Source: The Yorksire Post Tom Laverick suffered years of misery from hay fever until he tried acupuncture. Catherine Scott reports.
For Tom Laverick summer had become a season he dreaded from being a child. Debilitating hay fever caused him problemsin lcuding nosebleeds, throughout his childhood and into adulthood. “I’ve suffered severely with hay fever since I was a young child,” explains Tom. “I kept being told I would grow out of it as I got older but I didn’t and, if anything, it probably worsened. “ He tried all conventional remedies from tablets, nasal sprays and eye drops. “I even tried home remedies such as eating local honey, and nothing worked.” Tom then started working at the in ICT at the Northern College of Acupuncture in York. “Both my parents have had acupuncture over the last couple of years and had success with it so, having exhausted all of the previous treatments, I decided to try it for myself last summer when the symptoms flared up.” Tom started by having one treatment per week for three weeks to combat the symptoms he was suffering from at the time. He then had three monthly treatments to keep the symptoms at bay for the rest of the summer. “I’d been told acupuncture didn’t hurt but still felt sceptical at the thought of all the needles. I honestly didn’t feel any pain though and actually found it to be a very relaxing experience. “The success of the treatment was incredible. After just a couple of treatments, I was hardly suffering at all and it was first time I’d gone through an entire summer without having any nose bleeds, something I regularly suffered with at the height of the summer months. “It really did feel like the first time I’d actually been able to enjoy summer rather than dreading it and wanting to hide inside. If anyone suffers from hay fever, I really couldn’t recommend acupuncture highly enough.” NCA Principal, Richard Blackwell said: “I’m delighted to hear of the impressive improvement in Tom’s hay fever symptoms. “Many hay fever sufferers benefit from acupuncture, although Tom responded exceptionally well after a small number of treatments. Tom’s experience is backed up by a recent review of the research evidence published by Australian researchers which concluded that allergic rhinitis, which includes hay fever, is one of eight conditions for which there is strong evidence of acupuncture’s effectiveness.” The Acupuncture Evidence Project, a large scale review of the evidence base, completed in Australia in 2017, has found acupuncture to be effective for 177 conditions. Most notably mentioned are: chemotherapy induced side effects, seasonal allergies, chronic low back pain, migraine prevention, chronic headaches, knee osteoarthritis and post-operative nausea and pain. It is thought that acupuncture may have evolved from the practise of bloodletting which was common to nearly all primitive cultures, China being no exception. Medial texts from the Han Dynasty (200 BC) show detailed pictures of the vascular system, and the Nei Jing, a classical text on Chinese Medicine, indicates the transition from bleeding an area to needling a specific point. Western medical acupuncture is the use of acupuncture following a medical diagnosis. It involves stimulating sensory nerves under the skin and in the muscles of the body. This results in the body producing natural substances, such as pain-relieving endorphins. It’s likely that these naturally released substances are responsible for the beneficial effects experienced with acupuncture. A course of acupuncture usually creates longer lasting pain relief than when a single treatment is used. Traditional acupuncture is based on the belief that an energy, or “life force”, flows through the body in channels called meridians. This life force is known as Qi (pronounced “chee”). Practitioners who adhere to traditional beliefs about acupuncture believe that when Qi doesn’t flow freely through the body, this can cause illness. They also believe acupuncture can restore the flow of Qi, and so restore health. While it’s common knowledge that acupuncture is useful for pain, many people are unaware that it is also beneficial for mental-emotional conditions such as stress, anxiety and depression. Acupuncture Awareness Week takes place from from March 6 – 12. Supported by the British Acupuncture Council; AAW aims to better inform people about traditional acupuncture, as well as raise awareness of its benefits. The Northern College of Acupuncture in York, is the only institution of its kind in the North of England. Its founder, Dr Hugh MacPherson, is the UK’s first ‘Professor of Acupuncture Research’ at the University of York. For more information visit https://chinese-medicine.co.uk Struggling to wake up full of energy in these dark winter mornings? Hitting the snooze button too often and snuggling back under the duvet?
This is true of many of us this time of year and often we blame our bodies, feeling they are somehow letting us down as we wonder at our lack of energy. So maybe we need to look at what is going on from a different perspective? The perspective of Chinese medicine … Chinese medicine is thousands of years old and based on principles developed from living at one with nature and the environment. One of its main principles is learning to live in harmony with the seasons. By understanding and appreciating the energetic shifts in both ourselves and nature, it provides us with ways and means to help us get the most out of each season as we go through the year. So what does the winter landscape tell us about nature and energy? Looking outside the landscape is stripped back and bare, nature at its slowest and quietest. Winter, therefore, was considered a time for us to slow down, to conserve and build our energies for the year ahead, and a time for inward reflection. For example, in ancient, agricultural China it was normal to go to bed not long after dark and get up with the morning light - living at one with nature. There were many reasons for this apart from just light, such as conserving energy as food supplies were perhaps limited, keeping warm etc. Of course, this is no longer how we live as we have the ability to put more active hours into our days, have a plentiful supply of food and warmth at the touch of a button. Thankfully, because of our modern way of life, many people love the winter and feel no less energetic at this time than at any other time. For others, however, the winter months can have a real impact on their sense of well-being. So how can we optimize our energy through the winter? Resting – get plenty of sleep, enjoy early nights and try to get a lie in on weekends. Conserving energy – try to reduce stress as it greatly depletes energy. There are many things we can do to cope with stress in ways that support the conservation of our energy like yoga, meditation and walking. Winter is not the time of year to be doing exercise that makes you sweat – there’s the rest of the year for that! Building energy – eating seasonal foods such as root vegetables, seeds, nuts and dried fruit. Ideal dishes are slow cooked, warming foods such as soups and casseroles. Avoid too many raw, cold foods such as salads during the winter, and also avoid iced drinks. Reflection – winter is an ideal time for inward reflection, to consider what we want out of our lives, how we hope achieve these goals and for making plans for the year ahead. Spring is just around the corner and this is the time for energy expenditure as we implement our plans! There are a few weeks of winter left so go with the energetic flow, get some rest, eat hearty, warming foods and don’t feel guilty as you pull the duvet back over your head and enjoy your weekend lie in! It’s only natural. With the festivities of Christmas and New Year over, many of us feel out of sorts as we face the long dark month of January. Why not put the spring back into your step and book an appointment for Reflexology? Deeply relaxing and soothing, it can get you back on your feet! Not only that but if you book in with me at Neal's Yard, Stamford on any Tuesday in January, then a beautiful presentation box of their new organic revitalise shower gels is yours FREE! Call me on 07737 172939 or call the store on 01780 752505 to book your appointment.
Going through the menopause will be a very different experience for each woman, however, hot flushes and night sweats, are one symptom that many women have to endure. Although HRT is known to help relieve this particular symptom, it does come with certain potential side effects. Due to these, many women search out more natural therapies to help ease them through these difficult symptoms.
A recent randomized controlled study by Gozuyesil E, Baser M (2016), published in Complementary Therapies in Clinical Practice, looked at the effect of foot reflexology applied to women aged between 40 and 60 on vasomotor complaints and quality of life. 120 women were randomly assigned to an experimental group or control group. The experimental group received foot reflexology whilst the control group received a non-specific foot massage. The results showed a decrease in symptoms in both groups, however, there was a statistically significant improvement found in the reflexology group. The conclusion being that reflexology may help in decreasing hot flushes and increasing the quality of life in menopausal women. Researchers find Traditional Chinese Medicine (TCM) modalities including acupuncture, tuina, and moxibustion effective for the treatment of pain associated with osteoporosis. Conclusions reached across several studies delineate specific benefits resulting from the application of acupuncture. Acupuncture outperformed estrogen replacement therapy for bone pain reduction in women with osteoporosis. Related studies confirm the benefits of TCM therapies. Moxibustion (a warming technique employing the use of burning mugwort) at four key acupoints was found successful at regulating blood plasma estradiol levels.
Additional studies are consistent with these findings. Another recent study finds acupuncture combined with tuina (traditional Chinese medical massage) beneficial for bone metabolism. In addition, acupuncture outperformed drug therapy for the treatment of osteoporotic spinal compression fracture related pain. The aforementioned study confirms the analgesic effects for which acupuncture is renown. Finally, Chinese herbal medicine combined with acupuncture outperformed supplementation with calcium combined with miacalcine (calcitonin-salmon), a synthetic hormone used for the treatment of osteoporosis. Patients receiving herbs and acupuncture had greater bone mineral density improvements and greater reductions of pain, dizziness, and numbness than the supplement group. Let’s take a closer look at these important findings. Hematologic findings confirm the efficacy of TCM. Wu et al. performed moxibustion at acupoints DU4 (Mingmen), ST36 (Zusanli), UB20 (Pishu), and DU14 (Dazhui). They that this combination of acupoints increased the levels of estradiol in the blood plasma of elderly men and women. (1) Yue and Zeng compared acupuncture therapy to estrogen replacement therapy in 60 women with postmenopausal osteoporosis. They found that acupuncture was more effective in lowering the bone pain score, the osteoporosis symptom score, and the kidney deficiency symptom score than estrogen replacement therapy. (2) Wang et al. compared two protocols in 64 patients with age related osteoporosis due to calcium calcium deficiencies. The first therapeutic protocol combined acupuncture and tuina (Chinese medical massage); the second protocol combined oral administration of calcium carbonate and vitamin D3 into a therapeutic regimen. Biochemical indices of bone metabolism improvements were similar in both test groups, indicating that acupuncture plus tuina provides many of the benefits afforded by supplementation. Biomechanical indices demonstrated significant improvements. The acupuncture and tuina combination caused a direct improvement measured in the lumbar lordosis index and sacral inclination angle changes. This demonstrates therapeutic effects on the lumbar spine. (3) Specific acupuncture protocols have been tested for their efficacy in enhancing osteoporosis drug therapies. Zhang et al. conclude that abdominal acupuncture combined with drug therapy is more effective than drug therapy alone for the treatment of pain caused by osteoporotic spinal compression fractures. Furthermore, Zhang et al. find abdominal acupuncture points especially effective when compared with the application of local acupuncture points. (4) In a similar study, Yuan et al. tested the efficacy of electroacupuncture and herbs (Jiawei Shentong Zhuyu decoction) in conjunction with a protocol of calcium carbonate, vitamin D, and calcitonin-salmon supplementation. Patients in the treatment group receiving the TCM protocols combined with supplements had a 92.5% total effective rate for the relief of pain, numbness, and dizziness. Additionally, functional improvement of walking was significant. Patients receiving only supplements achieved an 80% total effective rate. Objective measurements revealed something very important. Bone mineral density improved more significantly in the TCM plus supplements group than in the group receiving only supplements. (5) Laboratory findings are consistent with the aforementioned clinical trials. Zhao et al. determined that moxibustion combined with acupuncture has an additive or synergistic effect when combined with drug therapy for regulation of estradiol levels in the blood. (11) Liu et al. found that treatment with acupuncture and moxibustion on acupoints including UB11 (Dazhu), DU14 (Dazhui), and Mingmen (DU4) had a similar effect as treatment with estradiol in regulating levels of estradiol and parathyroid hormone (PTH). (12) Li et al. demonstrated that acupuncture along the governor meridian (Du Mai) can increase bone density. (13) Lab studies conducted by Zhou et al. show that electroacupuncture improves bone mineral density and prevents bone loss. (14) Based on the findings cited here, we would like to see a large, multi-centered controlled clinical trial focusing on subjective and objective improvements through the use of TCM for patients with osteoporosis. Blood samples, imaging technology, and biomechanical testing are adequate measures in human clinical trials to avoid any need for continuance of animal experimentation. Further, establishing accepted protocols for integrative medicine approaches to osteoporosis care are of paramount importance. At the Healthcare Medicine Institute (HealthCMi), we are encouraged by the current research and look forward to seeing new research focusing on practical methods of TCM protocol integration into standard care settings. References: (1) Wu ZC, Wang LL & Xu LF et al. (1996). Effect on plasma testosterone and estradiol of old people. Chinese acupuncture & moxibustion. (8): 27-28. (2) Yue YR & Zeng ZP. (2001). The contrastive study is between before and after acupuncture for estrogen in postmenopausal osteoporosis. China medical herald. 20(10): 641. (3) Wang T, Pang L, Huang H, Wang WY. Zhongguo Zhen Jiu journal. 2012 Jan; 32(1):13-6. Observation on influence of bone metabolism biochemical indices of senile osteoporosis treated with distant acupuncture and nearby tuina). Institute of Acupuncture and Moxibustion, China Academy of Chinese Medical Sciences, Beijing, China. (4) Zhang, W., Qiu, X. Y. & Wang, J. (2015). Clinical study on abdominal acupuncture for osteoporotic vertebral compression fracture. Journal of Acupuncture and Tuina Science. 13(4). (5) Yuan LM, Li YM, Chen LM, Lei XH & Jia SJ. (2015). Therapeutic Effect on Primary Osteoporosis Treated by Electro-acupuncture Combined with Jiawei Shentong Zhuyu Decoction. Journal of Clinical Acupuncture and Moxibustion. 31(8). (6) Jin, Yuelong, Lianping He, Quanhai Wang, Yan Chen, Xiaohua Ren, Hui Tang, Xiuli Song, Lingling Ding, Qin Qi, Zhiwei Huang, Jiegen Yu, and Yingshui Yao. "Serum Calcium Levels Are Not Associated with Coronary Heart Disease." Vascular Health and Risk Management. Dove Medical Press, 3 Sept. 2013. Web. 16 Sept. 2016. (7) Morley, Paul, James Whitfield, and Gordon Willick. "Parathyroid Hormone An Anabolic Treatment for Osteoporosis." CPD Current Pharmaceutical Design 7.8 (2001): 671-87. Web. (8) Chinese Medical Association of Osteoporosis and Bone Mineral Disease Branch. Treatment Guidelines of Osteoporosis. (2011). Chinese Journal of Osteoporosis and Bone Mineral Research. 4(1): 2-15. (9) Meng XW. (2012). The risk factors and assessment of primary osteoporosis. Journal of Diagnostics Concepts & Practice. 11(1): 1-4. (10) Office of the Surgeon General (US). "Bone Health and Osteoporosis: A Report of the Surgeon General." The Basics of Bone in Health and Disease. U.S. National Library of Medicine, n.d. Web. 16 Sept. 2016. (11) Zhao Yingxia, Yan Zhenguo, Shao Shuijin. (1999). The effect of acupuncture and moxibustion on experimental osteoporosis. Chinese acupuncture and moxibustion. (19): 301-303. (12) Liu XX, Wu Mx, Wu BH et al. (2000). The effect of acupuncture and moxibustion on osteoporosis experimental and clinical studies. China journal of orthopaedics and grammatology. 13(9): 519-521. (13) Li Y, Xu GS, Liu GX et al. (2006). The influence of acupuncturing Du Meridian to cure osteoporosis rats model serum cytokines and bone mineral density. Journal of Anhui TCM College. 25(6): 27-29. (14) Acupunct Med 2012;30:37-43 doi:10.1136/acupmed-2011-010114. Electroacupuncture prevents ovariectomy-induced osteoporosis in rats: a randomised controlled trial. Jun Zhou, Shiju Chen, Hua Guo, Lu Xia, Huifang Liu, Yuxi Qin, Chengqi He. There isn’t much research to support this ancient practice, but athletes love it anyway.
08/08/2016 06:53 pm ET | Updated 1 day ago Anna Almendrala Senior Healthy Living Editor Michael Phelps won his first gold of the Rio Olympics on Sunday with telltale cupping marks on his back and shoulders, putting him in the company of alternative health-loving celebrities like Jennifer Aniston, Gwyneth Paltrow and Lena Dunham. But Phelps isn’t the only athlete in Rio with the circular bruises ― several other American Olympians have found healing and relief in this ancient traditional therapy. Though cupping made an appearance at the 2008 Games in Beijing as well, this may be the first time it’s found such wide appeal among the members of Team USA. Cupping, which has roots in ancient Egypt, the Middle East and China, is said to increase blood flow where it’s applied, and stimulate the body’s “natural energy,” or qi. Sections of skin are suctioned for several minutes, leaving round purple or red bruises on the surface. But how does this therapy stack up when tested scientifically? In the case of athletes, there are no studies that seem to test cupping’s ability to enhance athletic performance. Other elite swimmers, including Phelps’ teammate Nathan Adrian, have said cupping is simply a good alternative to massage therapy. However, there is research that suggests cupping may be effective in treating more than just an athlete’s sore muscles. Several studies have investigated whether cupping can be a helpful or complementary therapy for chronic pain, migraines, and facial conditions. These studies show that compared to other therapies, cupping may be as or more effective at relieving certain medical conditions. But they should all be taken with a grain of salt, because none have cleared the highest bar of therapeutic research: testing the intervention (in this case, cupping) against a placebo control. Having a placebo treatment would separate the effects of cupping from a study participant’s beliefs about its effectiveness, allowing for a more accurate measure of any medicinal properties. The reason there are no placebo control groups in cupping studies is that scientists simply haven’t found a way to create a convincing placebo intervention for cupping, notes the Mayo Clinic. Researchers at the University of Western Sydney’s Centre for Complementary Medicine Research found in 2012 that cupping, in combination with other traditional Chinese medicines or pharmaceutical medicines, appeared to be more effective at treating things like acne, facial paralysis, and herpes zoster than other traditional or pharmaceutical treatments alone. They came to this conclusion after reviewing 135 randomized controlled trials, although they do concede in the report that most of the studies had a high risk of bias. Cupping may also provide some benefit when it comes to pain. A 2011 study of 7 randomized controlled trials found that people experienced significant pain reduction with cupping compared to typical treatments like pharmaceutical painkillers, anti-viral medications or heat pads. But like the 2012 meta-analysis, the researchers for this study also pointed out that most of the trials had a high risk of bias and weak methodology. They also noted that there may be a publishing bias, in that researchers only bother to publish positive results about cupping and other traditional therapies, which doesn’t allow others to examine and assess any possible negative effects. Those with chronic headaches may also benefit from cupping. A 2008 Iranian study on the effects of “wet cupping,” which combines suction with controlled bleeding of the suctioned skin, found that participants experienced an average of 66 percent decrease in pain severity for up to three months after a wet cupping treatment, as well as 13 fewer days of headaches per month. Does it matter? Marcus Williams, a physical therapist at the Ohio State University Wexner Medical Center, has been using cupping on his clients for about two years now. While he and his colleagues continue to keep an eye on cupping research as it’s published, they’re confident that cupping is a safe, non-invasive procedure they can use on clients who are suffering from soreness or chronic pain. Unlike traditional physical therapy techniques like massage, which applies force to muscles or tendons, cupping pulls skin and tissue away from the body, which is a unique way of relieving stress, Williams explained. “We thought that was intriguing from the standpoint of patients who come in with tendinopathy or tendonitis,” Williams said. “If we can decompress and unload some of the structures that are getting overworked, it can be beneficial.” Anecdotally, Williams has found that cupping is an effective way to relieve soreness or pain and will continue to use it “when appropriate,” and especially when other therapies fail to relieve the pain. So, should you try cupping? It’s going to take high-quality trials with placebo control groups to turn up more reliable information about the effects of cupping. But it doesn’t look like Phelps or any other athlete is going to wait for those results when they’ve got a medal to win. If you have muscle soreness or chronic pain and traditional therapies have failed, it doesn’t hurt to try suctioning up a few square inches of skin to see if you can get some relief. But the jury’s still out on whether the suctioning actually helps, or if the placebo effect from the treatment is so strong that it can transform your perception of pain. Scientific research confirms that acupuncture is safe and effective for preventing and alleviating migraine headaches.
Studies demonstrate that acupuncture is an effective method for relieving migraines. Small clinical studies and large scale meta-analyses confirm the efficaciousness of acupuncture. Additional research demonstrates that acupuncture is an effective alternative to medications for the treatment of migraines with acupuncture demonstrating superior positive patient outcomes in both short and long-term results. A large body of scientific evidence demonstrates that acupuncture is effective for the relief of migraines. From small clinical studies to large scale analyses, acupuncture has been proven both safe and effective. In addition, researchers find true acupuncture more effective than sham acupuncture. University of Louisville (Kentucky) doctors published findings in Pediatric Emergency Care. Their approach was to employ auricular acupuncture for the purposes of evaluating the “utility and adverse effects of auricular acupuncture in the treatment of pediatric migraines in the ED [emergency department].” The doctors note, “There were no adverse events associated with any patient during the study.” The doctors conclude, “With all subjects showing improvement or resolution of migraine headache, this pilot study introduces an alternative intervention to pediatric migraine management. . . . auricular acupuncture seems to be a valid alternative.” Dr. Graff, MD and Dr. McDonald, MD (University of Louisville) recommend additional research based on their findings. Their study was limited by sample size and the use of a relatively non-invasive type of auricular acupuncture employing the use of tiny auricular semi-permanent gold needles. The doctors add, “Auricular acupuncture seems to be well tolerated in children and adolescents with migraines. This experimental protocol provides a unique approach to the pediatric patient with an acute migraine in the ED.” RMIT University and Royal Melbourne Hospital researchers find acupuncture effective for the relief of migraines (Wang et al.). They note, “Acupuncture can be used as alternative and safe prophylaxis for frequent migraine. Our recommendation is that practitioners treat migraine sufferers twice per week for at least eight weeks.” Their controlled study documents that sham acupuncture does not produce the significant positive patient outcomes as in true acupuncture. The researchers note that “more participants in the RA [real acupuncture] group used less pain killers as relief medication than in the SA [sham acupuncture] group” at the end of the treatment regimen. In addition, the total number of days with a migraine was significantly lower in the real acupuncture group as compared with the sham acupuncture group. Wang et al. document that 73% of real acupuncture patients had a 50% or greater reduction in the number of days with a migraine whereas the sham acupuncture group had a 29% reduction. The researchers note, "The present trial showed that acupuncture was effective in reducing migraine days, as well as effecting a reduction of medication consumption and improvement in quality of life, when compared with sham acupuncture." They add that the “results demonstrated that manual acupuncture can be an effective and a safe prophylaxis for frequent migraine sufferers.” The primary acupuncture points used in the study included the following:
The supplementary acupuncture points based on differential diagnostic pattern variations included the following:
MRI studies are consistent with the aforementioned migraine research. MRI research demonstrates that acupuncture “induce[s] different cerebral glucose metabolism changes in pain-related brain regions and reduce[s] intensity of pain” for patients with migraines. In a randomized controlled PET-CT neuroimaging investigation, acupuncture was found effective for the alleviation of migraine pain. The researchers documented that acupuncture raised brain glycometabolism in specific regions: middle temporal cortex, orbital front cortex, middle frontal gyrus, angular gyrus, post cingulate cortex, precuneus, middle cingulate cortex. Simultaneously, acupuncture lowered glycometabolism in the specific brain regions of migraine patients: parahippocampus, hippocampus, fusiform, postcentral gyrus, cerebellum. The study demonstrates that different acupuncture point selections caused predictable and repeatable changes in brain glycometabolism. Acupuncture point specificity was confirmed using MRIs, i.e., specific acupuncture points have specific effects on brain responses and related treatment outcomes. In other research, Tianjin University of Traditional Chinese Medicine researchers achieved a 100% total effective rate with an 88.6% complete recovery rate for the treatment of migraines with acupuncture and cupping. The primary acupuncture points used in the study included:
Cupping was applied to back shu (beishu) acupuncture points. Acupuncture was applied twice per week for eight continuous weeks. Needle retention time was twenty minutes per session and manual reinforcing and reducing techniques were applied. When the researchers tried the treatment protocol without cupping and acupoint CV17, the total effective rate dropped from 100% to 94.3% and the complete recovery rate dropped from 88.6% to 62%. The findings suggest that cupping and acupoint CV17 have important clinical benefits for patients with migraines. Additional research finds acupuncture more effective than valproic acid for the treatment of migraines (Facco et al.). In the study, acupuncture patients required less rizatriptan and had significantly lower pain intensity levels due to migraines than valproic acid patients. Acupuncture patients had no adverse side effects and valproic acid patients had a 47.8% side effect rate. Zhang et al. determined that the frontal and temporal lobes have “decreased functional connectivity” in migraine sufferers. Their MRI investigation demonstrates that acupuncture restores functional connectivity in those regions. After a four week course of acupuncture therapy, migraine sufferers “showed significantly increased functional connectivity in the bilateral superior frontal gyrus, medial frontal gyrus, precuneus, inferior parietal lobule, posterior cingulate cortex, cingulate gyrus, superior temporal gyrus, middle temporal gyrus, and supramarginal gyrus as compared with before acupuncture treatment.” In addition, the researchers concluded that acupuncture decreased the frequency and duration of migraine attacks after a four week course of acupuncture care. Guo et al. find acupuncture more effective than flunarizine hydrochloride for controlling migraines. In their investigation, acupuncture combined with tuina had a total effective rate of 93.8% whereas flunarizine hydrochloride achieved a 63% total effective rate. In addition, patients receiving acupuncture with tuina had significantly fewer relapses than the patients taking the drug. As a result of the findings the researchers conclude, “Combining electroacupuncture and local tuina can obtain better effect and lower relapse rate than oral Flunarizine Hydrochloride capsules in migraine patients.” Lin et al. conducted a randomized controlled trial of eighty-seven migraine patients. The following acupuncture points produced a 95.2% total effective rate measured six weeks following acupuncture and 88.1% measured three months following acupuncture treatments:
Scott et al. conclude that acupuncture is “of comparable efficiency to several proven drug therapies for the treatment and prevention of migraine[s].” The meta-analysis conducted by Scott et al. involved the investigation of twenty-five randomized controlled trials involving a sample size of 3,004 migraine sufferers. Given these and the aforementioned findings, the consensus of modern research is that acupuncture is both safe and effective for the treatment of migraines. References: Graff, Danielle M., and Mark J. McDonald. "Auricular Acupuncture for the Treatment of Pediatric Migraines in the Emergency Department." Pediatric Emergency Care (2016). Wang, Yanyi, Charlie Changli Xue, Robert Helme, Cliff Da Costa, and Zhen Zheng. "Acupuncture for Frequent Migraine: A Randomized, Patient/Assessor Blinded, Controlled Trial with One-Year Follow-Up." Evidence-Based Complementary and Alternative Medicine 2015 (2015). Yang, Jie, Fang Zeng, Yue Feng, Li Fang, Wei Qin, Xuguang Liu, Wenzhong Song, Hongjun Xie, Ji Chen, and Fanrong Liang. "A PET-CT study on the specificity of acupoints through acupuncture treatment in migraine patients." BMC complementary and alternative medicine 12, no. 1 (2012): 1. Jin SS, Du YZ, Han L, Liao C & Gu WL. (2015). Observations on the Efficacy of Acupuncture at Point Shanzhong (CV17) plus Cupping on Back-Shu Points in Treating Migraine. Shanghai Journal of Acupuncture and Moxibustion. 34(3). Facco, E., et al. "Acupuncture Versus Valproic Acid In The Prophylaxis Of Migraine Without Aura: A Prospective Controlled Study." Minerva anestesiologica (2013). Zhang, Yong, Kuang-shi Li, Hong-wei Liu, Cai-hong Fu, Sheng Chen, Zhong-jian Tan, and Yi Ren. "Acupuncture treatment modulates the resting-state functional connectivity of brain regions in migraine patients without aura." Chinese Journal of Integrative Medicine (2015): 1-9. Guo, Qing, Yu Hua, Hai-qin Wang, Ying Li, and Quan Ji. "Therapeutic effect observation on combining electroacupuncture and tuina for migraine." Journal of Acupuncture and Tuina Science 12, no. 3 (2014): 174-179. Lin, X. M., X. Yao, and Z. Di. "[Acupuncture at" Siguan" combined with Gallbladder Meridian acupoints for migraine: a randomized controlled trial]." Zhongguo zhen jiu= Chinese acupuncture & moxibustion 34, no. 10 (2014): 947-950. Scott SW, Deare JC. Acupuncture for migraine: a systematic review. ‘Aust J Acupunct Chin Med’ 2006;1(1):3-14). Individualized treatment with acupuncture in a primary care setting provided patients with fibromyalgia with pain relief compared to patients who received a placebo treatment, and the effects were persistent at 1 year, according to researchers in Spain.
Researchers studied data from 162 women with fibromyalgia who participated in the trial. Patients were aged 52.8 years, mean, with a mean disease duration of 70 months. A rheumatologist provided the diagnosis to 109 of the patients. All patients met 1990 American College of Rheumatology criteria for fibromyalgia and were naïve to acupuncture. Patients were excluded in the presence of a chronic pain condition unrelated to fibromyalgia, the use of anticoagulants or opiates, pregnancy or nursing, or pending occupational litigation related to fibromyalgia. Patients were evaluated using the Fibromyalgia Impact Questionnaire (FIQ), the Hamilton Depression Rating hetero-evaluation Scale (HDRS), SF-12, pain on a VAS, tender point count, and 114 patients completed a questionnaire item about family structure. Patients were evaluated at baseline (T0), 10 weeks (T1), 6 months (T2) and 12 months (T3) after they were randomly assigned to a treatment or sham treatment group. The acupuncture treatment group (n = 80) received acupuncture based on a previously established algorithm associated with traditional Chinese medicine principles. The sham acupuncture or placebo group (n = 82) received an application of guide tubes used in acupuncture to the dorsal and lumbar regions with the needles removed. Both groups received 20 minutes of treatment once a week. At T1, pain on a VAS was reduced in the treatment group by 41.2% and in the sham group by 27.1%. At T3, pain relative to baseline was reduced by 19.9% in the treatment group and in the sham group by 6.1%. The FIQ scores at T1, T2 and T3 were improved by 35.9%, 25% and 22.2%, respectively, in the treatment group compared to 24.5%, 11.2% and 4.9%, respectively, in the sham group. The fatigue domain of the FIQ was improved in the treatment group at T1 by 32.8% compared to 19% in the sham group. The anxiety domain in the treatment group was improved by 31% compared to 17.8% in the sham group, and depression scores improved in the treatment group by 33% compared to 18.5% in the sham group. Improvements favorable to the treatment group persisted at later time points, although at a smaller effect, according to the results. The relative difference in pain intensity after adjusting for tender pressure points and total FIQ score improved by 14.4% in the treatment group compared to the sham group. The researchers cautioned in their study about how these findings are interpreted because a greater quantity of antidepressants were utilized at the final time point and that may affect the results. – by Shirley Pulawski Disclosure: The researchers report no relevant financial disclosures. Vas J, et al. Acupunct Med. 2016;doi:10.1136/acupmed-2015-010950. Acupuncture alleviates depression and insomnia. Research published in the Shanghai Journal of Acupuncture and Moxibustion (Ye et al.) finds acupuncture 90% effective in improving total sleep duration and sleep quality for patients with depression. Alleviation of insomnia directly correlated to improvements in the mental and physical health of study participants. Acupuncture treatments lowered relapse rates and produced similar clinical results as antidepressants. Notably, acupuncture did not produce any adverse effects.
Two groups were compared. Group one received acupuncture and group two received oral tablets of mirtazapine, an antidepressant drug. Acupuncture therapy achieved a 90% total effective rate and mirtazapine therapy achieved a 92.5% total effective rate. Common mirtazapine adverse effects include dizziness, drowsiness, vision changes, weight gain, increased appetite, and constipation. No adverse effects occurred in study participants receiving acupuncture. Insomnia due to depression, termed depressive insomnia in Traditional Chinese Medicine (TCM), is characterized by difficulty falling asleep, dream disturbed sleep, generalized insomnia, and severe emotional fluctuations. Additional symptoms include major depression, loss of appetite, exhaustion, chest tightness, manic states, pain of the hypochondriac region, and excessive pessimism. Hamilton Depression Rating Scale (HAM-D) results measured demonstrative improvements in both the acupuncture and drug therapy patients. The acupuncture group demonstrated a 9.7% HAM-D score improvement within one month of treatment. The HAM-D score improved by 36.2% within three months. The drug group demonstrated a HAM-D score improvement of 15.9% within one month and 32.5% within three months. The total effective rate was determined by adding all patients with 30% – 100% clinical improvements. The acupuncture group achieved a 90% total effective rate. The drug therapy group achieved a 92.5% total effective rate. The drug therapy group received 20 mg of mirtazapine tablets orally at a rate of once per day for three months. The acupuncture group received acupuncture treatment sessions every other day. An exception was made for extreme cases of depressive insomnia; these patients received acupuncture at a rate of once per day. Treatments were applied over a three month period. The patients received a semi-protocolized acupuncture point prescription comprised of a set of primary acupuncture points for all patients and a set of secondary acupuncture points for specific differential diagnostic conditions. The primary acupoints were
Secondary acupoints were administered when one of two of the following conditions were diagnosed. For patients with the TCM diagnosis of liver qi stagnation, Taichong (LV3) and Yanglingquan (GB34) were added. For patients with heart and spleen related disorders, Zusanli (ST36) and Jianshi (PC5) were added. Manual acupuncture stimulation was applied to the needles to elicit deqi followed by a thirty minute needle retention time. During the needle retention period, manual needle stimulation was applied every ten minutes using lifting and thrusting techniques for sedation and tonification. The researchers conclude that acupuncture significantly improves sleep time and sleep quality while improving the overall mental and physical health of patients. No adverse effects occurred. Moreover, acupuncture reduced the relapse rate for depressive insomnia. Lin et al. had similar findings. Their research finds acupuncture points Lieque (LU7) and Zhaohai (KD6) potent clinical tools in the fight against generalized anxiety disorder (GAD). Lin et al. note that “a number of Meta analysis and system evaluations point out that acupuncture treatment has more advantages than drugs in the treatment of anxiety disorders….” Lin et al. add that acupuncture has a fast effective action, high compliance to the therapeutic regimen, and a relatively minimal risk of side effects compared with drug therapy. The research of Wang et al. confirms the aforementioned studies. Wang et al. conclude that acupuncture benefits sleep and reduces insomnia in a single-blinded, randomized, placebo-controlled investigation comparing acupuncture with sham acupuncture and estazolam, a benzodiazepine medication. True (verum) acupuncture produced significantly superior patient outcomes for insomnia patients including improvements in sleep quality and total sleep time. Primary acupuncture points used in the study were:
Acupuncture restored nighttime sleep and improved daytime energetics. Patients in the estazolam medication group experienced adverse effects including daytime drowsiness that typically ceased by midday. The researchers note, “The trial implied that verum acupuncture was superior in improving sleep quality and daytime functioning of primary insomnia compared with estazolam and sham acupuncture.” The researchers note that true acupuncture increased total sleep time and “improved sleep quality (SQ) and vitality (VT), decreased daytime dysfunction (DD) and sleepiness (ESS score).” References: Ye GC & Yan H. (2014). Therapeutic Observation of Acupuncture for Depressive Insomnia. Shanghai Journal of Acupuncture and Moxibustion. 55(6). Observation on the mechanism of acupuncture treatment for generalized anxiety disorder using Lieque (LU7), Zhaohai (KI6) as the main acupoints. Lin, Chuhua; Zhao, Xiaoyan; Liu, Xing; Fu, Wenbin. Bioinformatics and Biomedicine (BIBM), 2013 IEEE International Conference on. 18-21, 12-2-13. Lin-Peng Wang, Guo, Jing, Cun-Zhi Liu, Jie Zhang, Gui-Ling Wang, Jing-Hong Yi, Jin-Lian Cheng, and R. Musil. "Efficacy of acupuncture for primary insomnia: a randomized controlled clinical trial." Deutsche Zeitschrift für Akupunktur 57. |
Archives
December 2019
|